Positive vaccination messaging crucial for mothers

Dr Michael Gannon
Obstetrician & Gynaecologist at St John of God Subiaco Hospital.
Former President of the AMA (WA) and the Federal AMA

It has long been established that the most common reason for infants to present to their GP or an Emergency Department, to be admitted to hospital, or to be admitted in an Intensive Care Unit is bronchiolitis or pneumonia. Underlying this in a majority of cases is infection with Respiratory Syncytial Virus (RSV). By two years of age, nearly all children have been infected. The highly contagious virus typically causes symptoms similar to the common cold in immunocompetent adults. Earlier this year we saw the addition of maternal RSV vaccine to the National Immunisation Program (NIP).
 Mothers are invited to have the vaccination at 28-36 weeks of pregnancy, with subsequent production of antibodies crossing the placenta and passively immunising the fetus. This provides protection for the newborn for up to six months after the birth. While most reproductive-age women are unlikely to become ill themselves, it reduces the prospect of them passing on RSV infection to other vulnerable cohorts in the population, e.g. the grandparents.
Mothers are invited to have the vaccination at 28-36 weeks of pregnancy, with subsequent production of antibodies crossing the placenta and passively immunising the fetus. This provides protection for the newborn for up to six months after the birth. While most reproductive-age women are unlikely to become ill themselves, it reduces the prospect of them passing on RSV infection to other vulnerable cohorts in the population, e.g. the grandparents.
In my experience, the novel vaccine has proved acceptable to the vast majority of patients. There is no problem receiving the vaccine at the same time as Pertussis vaccination and/or Influenza vaccination.
Infants born to mothers who have inadvertently missed out on Abrysvo, or for any reason have a contraindication, can be vaccinated directly with Beyfortus (Nirsevimab).
These are exciting developments. Antenatal (passive) immunisation is acceptable to the vast majority of pregnant women. It has been consistently shown that positive messaging about the benefit or risk of vaccination from trusted antenatal care providers is an important part of the mothers’ decision making.
In my individual clinical practice, I have always strived to remove barriers to pregnant women receiving these vaccines. I see it as a very important part of the antenatal care I deliver to my patients. A patient who receives evidence-based advice on the safety of vaccination in pregnancy is not going to refuse the schedule of vaccines their newborn is offered under the NIP.
Do not forget this is a group of patients that collectively denies themselves perfectly safe things like caffeine, paracetamol and medium-rare red meat.
“ A patient who receives evidence-based advice on the safety of vaccination in pregnancy is not going to refuse the schedule of vaccines their newborn is offered under the NIP.
It is essential that whether patients see a GP, an obstetrician or a midwife, they receive evidence-based and positive information about the benefits of antenatal vaccination.
I find vaccine refusal completely exhausting. Vaccine hesitancy occupies a lot of time in consultations, but it is so important that antenatal care providers take the time to explain the benefits of antenatal vaccination, in the same way they explain the benefits of other interventions – such as screening for Group B Streptococcal (GBS) colonisation, or antenatal administration of Anti-Rh(D) injections in prophylaxis against haemolytic disease of the fetus and newborn.
While far from being a new thing, the proliferation and effective encouragement of so-called non-standard birth plans seems to have grown in recent years. Why a mother would refuse an injection of Vitamin K in prevention of haemorrhagic disease of the newborn is beyond me. Nonetheless, I suspect issues like this will be a part of obstetric practice for the rest of my career.
I am very proud to have been involved in the then Telethon Kids Institute’s contribution to development and licensing of the Pfizer vaccine, Abrysvo. We are very fortunate to have researchers of the calibre of Professor Peter Richmond and Professor Chris Blyth working with us in Western Australia. Other vaccines to protect the mother and newborn will no doubt emerge in time. For now, we are stuck with intrapartum Penicillin to overcome the menace of potential invasive GBS septicaemia. The good work of researchers and clinicians must and will continue.
- The 2025 national RSV immunisation program for pregnant women and newborn babies hopes to keep 10,000 Australian babies out of hospital each year, according to the Immunisation Foundation of Australia.
- The WA Department of Health says Abrysvo and Beyfortus vaccinations will be available at participating maternity hospitals, general practices, Aboriginal medical services, and community health immunisation clinics. Community pharmacies will offer Abrysvo, but not Beyfortus.
- More information about the program in WA can be found at: health.wa.gov.au/Articles/N_R/2025-WA-Respiratory-Syncytial-Virus-RSV-Infant-and-Maternal-Immunisation-Program
- The REVIVE research study, funded by Perth Children’s Hospital Foundation, found that WA babies given Beyfortus under a State immunisation program last year were 88.2% less likely to be hospitalised with RSV. Vaccinated babies who were admitted with RSV were 60% less likely to require oxygen or assistance with their breathing.
Statewide total 2025*
1,630
5-Year YTD average 2021–2025 = 6696
Statewide aboriginal to non-aboriginal rate ratio (2025*)
3.3:1
rate per 100,000 population
Statewide male to female rate ratio (2025*)
0.8:1
rate per 100,000 population
Statewide RSV Notifications by quarter 2020-2025*
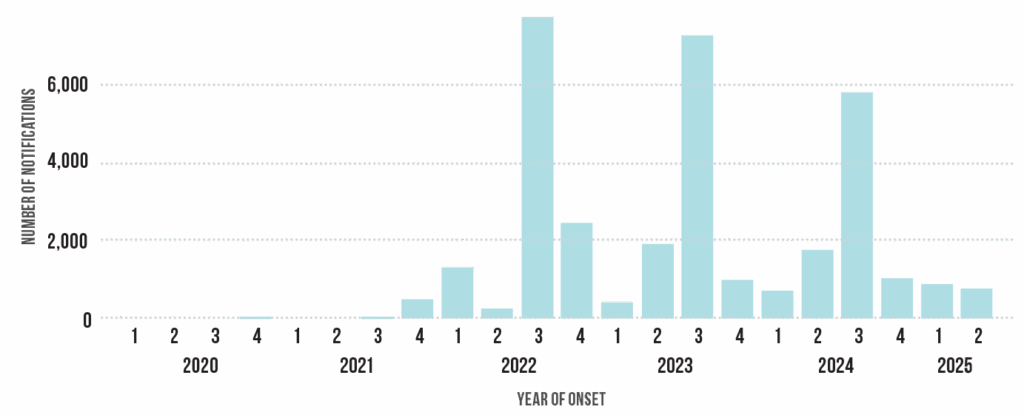
| Year | Number | Rate |
|---|---|---|
| 2020 | 1 | 0.04 |
| 2021 | 486 | 18.33 |
| 2022 | 11,360 | 435.47 |
| 2023 | 10,488 | 389.98 |
| 2024 | 9,245 | 341.37 |
| 2025* | 1,630 | 143.44 |
Respiratory syncytial virus (RSV) became a notifiable infections disease in August 2021




