Data in the driver’s seat
When paired with passionate clinical champions and interdisciplinary teamwork, data becomes a powerful agent of change

Kevin Trentino PhD
Manager, Research & Evaluation, Community & Virtual Care
East Metropolitan Health Service

The WA Patient Blood Management (PBM) Program is a standout example of international success. Launched in 2008 by the Department of Health, it has become a global benchmark for health systems – earning widespread recognition and establishing WA as a leader in the field.
The program’s outcomes are published in the journal Transfusion, with the 2017 manuscript1 ranking among its most accessed, cited and discussed articles. And for the data enthusiasts (you know who you are), the WA PBM story offers a compelling lesson that when used well, data isn’t just informative; it’s a powerful catalyst for change.
Consider just one of the many examples. Building on the work initiated at Fremantle Hospital, in late 2015 the Fiona Stanley Hospital’s (FSH) Department of Anaesthesia sought to establish a clinic for the screening and treatment of common preoperative conditions such as iron deficiency and anaemia.
Dr Hamish Mace, a consultant anaesthetist and part-time data enthusiast, took the lead on the initiative and later enlisted the support of Kylie Symons, a senior registered nurse, who would also go on to play a pivotal role. The reasons for setting up a clinic were intuitive – to enhance patient recovery after surgery and avoid unnecessary blood transfusions.
Predictably, there were obstacles.
The team did not have dedicated staff to lead the day-to-day work, or access to data to efficiently run the program and assess impact. This is when they engaged others – an interprofessional team which, in addition to perioperative specialists, included data analysts, IT, hospital management, and researchers.
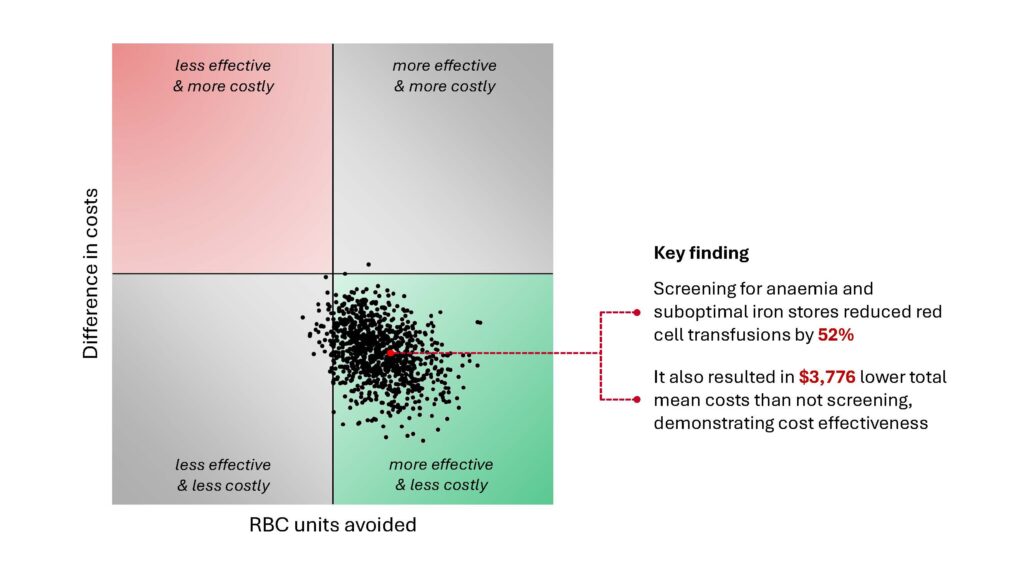
Fast forward four years (and much work later), the data generated by the program was published in several high-impact international journals. These publications included evaluations comparing economic and clinical outcomes to determine program value.
The result? Not only had the work started by the FSH Anaesthesia Department saved the health system money, but it also contributed to lower length of stay, less transfusion, and an increase in activity-based funding (Figure 1).
These outcomes had local and international impact, including at the World Health Organization level. The biggest impact, however, was that the data formed the glue for the successful business case to have a senior registered nurse position to manage the program – a role that continues to this day.

The Patient Blood Management Team at RPH with dedicated PBM Nurse Alun Thomas (far right).
For context, experts agree that a PBM nurse is considered essential to imbed patient blood management successfully and sustainably in day-to-day operations.
In summary, the data analysed and published contributed to re-investment into patient care, bringing benefits to the wider community. But, as is common with data, there were unexpected ripple effects.
Royal Perth Hospital (RPH) was also experiencing high transfusion rates among elective major surgery patients, highlighted by recent national benchmarked data. The data pointed to FSH as an exemplar with lower transfusion rates, and motivated communication between hospitals.
Unsurprisingly, a brief time later, RPH also created a senior PBM nurse position, which still exists to this day. An important lesson from the WA PBM example is the role of clinical champions and teamwork.
The “numbers have no way of speaking for themselves” (Nate Silver, The Signal and the Noise) and there are no unicorns. Successfully converting siloed and underutilised data into action requires the collaboration of interdisciplinary teams passionate about patient care.
The example presented is not an isolated case.
The East Metropolitan Health Service’s Health in a Virtual Environment (HIVE) program exemplifies the intersection of remote monitoring and AI, a space widely regarded as the future of healthcare. HIVE is a novel service that remotely monitors the continuous vital signs of high-risk inpatients located outside critical care areas.
Early results from the program are encouraging. In its first two and a half years, more than 7,500 patients were monitored for over 300,000 hours. This facilitated more than 10,000 clinical interactions between the remote and ward teams, with many occurring during high-risk periods such as weekends and after hours.

Kevin Trentino (centre) flanked by Kylie Symons and Dr Hamish Mace from FSH.
Among major surgical cohorts, the program has demonstrated its ability to save ICU beds and reduce hospital costs.
If data is power, the high-frequency physiological data routinely generated by the HIVE system can be a catalyst for transformative changes in care delivery. This is highly relevant to PBM and other patient care initiatives, of which the HIVE team have several exciting research projects underway.
For example, this high-frequency data is forming the building blocks of machine learning and AI-based algorithms to predict transfusion, post-operative bleeding, and other signs of clinical deterioration.
In healthcare, data is often seen as the quiet observer. It is collected, stored, occasionally consulted, and frequently underutilised. But, as these examples show, when paired with clinical champions and interdisciplinary teamwork, data becomes a powerful agent of change.
From reducing transfusions to predicting deterioration, the ripple effects are real and measurable. The challenge now is making the best use of what we already have to effectively shape the future of patient care.
______________
References available on request.




